Walk that walk!
Join me and some of the New York team on Saturday September 28th September for the JDRF walk. You can also donate here.
_______________________________________________________
My Story:
It was a week-long haze of blurry events which all came to a very clear diagnosis. On April 4th, 2011 I was told I had Type 1 Diabetes.
I was traveling home to San Francisco from a bachelorette party when I had the first indication that something was wrong. I was sluggish and exhausted and at 30 years old, I chalked it up to not being able to handle a long weekend of partying anymore! But the following morning, I couldn’t get out of bed. I had such severe muscle weakness that I could barely put one foot in front of the other and I couldn’t lift my arms over my head.
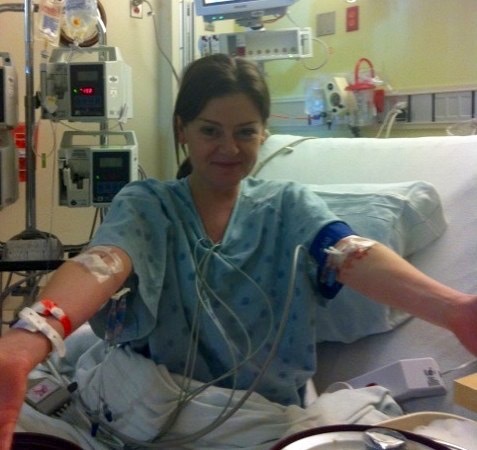
In the week that followed, a number of distinct events stood out. A doctor on multiple occasions misdiagnosed my symptoms and told me I likely had a virus that could take months to run its course. I remember dragging myself out of my apartment only to buy every sugary drink the corner store could sell me – despite how sick I felt, I was insatiably hungry and thirsty. I forced myself to go to work one day; my breathing was labored and my co-workers convinced me to leave and go back to the doctor. At this point that they finally began to connect the dots. They tested my blood sugar and it was in the 300’s (normal is 70-100). The doctor sent me home with a blood sugar meter and suggested I “do some push-ups” to bring my sugar down. Mind-blowing and incredibly inept medical advice, in retrospect. Thankfully, a dear friend intervened and took me to the Emergency Room where a urine test quickly confirmed a Type 1 Diabetes diagnosis. I was in Diabetic-Ketoacidosis (DKA), a potentially lethal outcome of T1D, at the time. I spent the next 4 days in the Intensive Care Unit, beginning insulin therapy and beginning to learn the treatment protocol what would become my “new normal”.
I was tossed back into the world, albeit with a vast personal and medical professional network, but largely left to my own devices to manage a disease that can be deadly if mismanaged or underestimated on any given day. Before my diagnosis, like the average person, I knew nothing about T1D. In the years since my diagnosis, my goal has been to create greater awareness and understanding of this disease. Its symptoms are not understood and often go unrecognized, and there is widespread public confusion over the difference between Type 1 and Type 2 diabetes, largely due to significant media coverage of Type 2 that brands it as a lifestyle disease related to unhealthy diet and exercise habits. However, Type 1 diabetes is not related to lifestyle factors and cannot be prevented or reversed. It is an auto-immune disease in which your body attacks your pancreas, destroying the cells that produce insulin. Insulin is a hormone that allows your body to use sugar from carbohydrates in the food that you eat for energy. Insulin helps keeps your blood sugar level from getting too high (hyperglycemia) or too low (hypoglycemia). Without it for an extended period of time, sugar builds up in your bloodstream and your body begins to burn fat and muscle for energy, which can be toxic and deadly if not treated. Type 1 diabetics require daily injections or infusions (via an insulin pump) of insulin to survive.
I’ve worn an insulin pump which helps calculate and deliver insulin based on my current blood sugar and carbohydrate intake. For a number of years, I’ve also worn another device called a Continuous Glucose Monitor (CGM) which places a small sensor under your skin to test your blood sugar every 5 minutes. This allows me to know my blood sugar at all times and treat appropriately without actually testing it on a meter – it’s been life changing. Ask anyone in the office – they often hear my phone or some device beeping incessantly – my warning system that alerts me to low blood sugar.
I find T1D an equally fascinating and frustrating disease. It’s not simply a matter of taking insulin to offset carbs that you eat. Illness, stress, sleep, exercise, pregnancy, temperature, dehydration – all of these are factors that impact your blood sugar and how your body uses insulin. Each day is like a new science experiment, walking a tightrope to achieve balanced blood sugar based on decisions related to all these factors. T1D is an invisible and “manageable” disease, which is both its beauty and its curse. No one would ever look at me and know I have a chronic disease. Yet I spend countless moments every day making calculated decisions related to this disease – How will this food impact my blood sugar? Will it drop while I exercise? Is something going to happen while I am in this meeting? How can I treat this severe low while managing my 3-year-old? I contemplate these things on my own 99% of the time, it can be a lonely disease! Yet I’m thankful every day that I lived the first 30 years of my life Type 1 Diabetes free, and I appreciate the knowledge, patience and empathy this disease has granted me.
For more information on the warning signs of T1D click here